Complete Guide to Virtual Psychiatric Treatment: Conditions, Medications, and What to Expect

Key Points:
- Virtual psychiatric treatment provides the same quality care as in-person appointments through secure, HIPAA-compliant video platforms
- Psychiatrists and psychiatric nurse practitioners can evaluate, diagnose, and prescribe medications for all major mental health conditions via telehealth
- Conditions treated include anxiety disorders, depression, bipolar disorder, ADHD, PTSD, eating disorders, psychosis, and many others
- Medication management happens entirely virtually including initial prescribing, monitoring, adjustments, and refills sent electronically to your pharmacy
- Virtual psychiatric appointments offer convenience, privacy, faster access, and eliminate travel barriers while maintaining clinical effectiveness
- Getting started is simple with flexible scheduling, same-day appointments available, and services accessible from any smartphone, tablet, or computer
What Is Virtual Psychiatric Treatment?
Virtual psychiatric treatment is mental health care provided by licensed psychiatrists or psychiatric-mental health nurse practitioners (PMHNPs) through secure video appointments instead of traditional in-person office visits.
The clinical services are identical to what you'd receive in a psychiatrist's office. The only difference is location. You connect with your provider from wherever you're comfortable (your home, office, car, or any private space) while they provide expert psychiatric care through a screen.
What Virtual Psychiatrists Can Do
Complete Psychiatric Evaluations: Your provider conducts comprehensive assessments of your mental health symptoms, history, and current functioning to make accurate diagnoses.
Medication Management: Psychiatrists and PMHNPs prescribe all psychiatric medications including antidepressants, mood stabilizers, antipsychotics, anxiety medications, ADHD treatment, and sleep medications.
Ongoing Treatment: Regular follow-up appointments to monitor medication effectiveness, manage side effects, adjust dosages, and ensure optimal treatment outcomes.
Therapy and Counseling: Many providers offer supportive therapy, cognitive behavioral techniques, and psychoeducation alongside medication management.
Specialized Services: Diagnostic testing, DNA genetic medication testing (GeneSight), bariatric surgery clearances, court-ordered mental health evaluations, emotional support animal letters, and more.
Coordination of Care: Collaboration with your therapist, primary care doctor, or other healthcare providers to ensure comprehensive treatment.
How Prescriptions Work Virtually
One of the most common questions people have is: "How do I get my medication if I never see the doctor in person?"
The answer is simple: electronic prescribing.
The Process:
During Your Appointment: Your provider evaluates your symptoms and determines which medication would be most helpful. They discuss the medication with you, including how it works, potential side effects, and what to expect.
Electronic Prescribing: Your provider sends the prescription electronically (e-prescribing) directly to the pharmacy of your choice. This happens instantly during or immediately after your appointment.
Pick Up Your Medication: You receive a text or call from your pharmacy when your prescription is ready. You pick it up just like any other prescription.
Refills: Request refills through your patient portal, secure messaging, or during follow-up appointments. Your provider sends refills electronically to your pharmacy.
Is Virtual Psychiatric Care Effective?
Extensive research shows that virtual psychiatric treatment produces outcomes equal to in-person care for most conditions.
The Evidence:
Patient Satisfaction: Studies consistently show 85-95% patient satisfaction with telepsychiatry, often higher than in-person care due to convenience and reduced anxiety about visiting medical offices.
Clinical Outcomes: Research demonstrates equivalent symptom improvement, medication adherence, and treatment success rates for virtual versus in-person psychiatric care.
Particularly Effective For:
- Medication management for depression, anxiety, ADHD, bipolar disorder
- Follow-up appointments and medication monitoring
- Patients with transportation barriers or mobility limitations
- People in rural areas without local psychiatric access
- Individuals with social anxiety who find in-person appointments stressful
What Virtual Care Can't Do: Virtual psychiatric treatment works extremely well for the vast majority of conditions, but some situations still require in-person evaluation:
- Patients experiencing severe psychosis who need immediate hospitalization
- Situations requiring physical examination beyond visual assessment
- Some emergency psychiatric situations requiring crisis intervention
For most people seeking psychiatric medication management, therapy, and ongoing mental health support, virtual care is not just adequate but often preferable.
If you're wondering whether virtual psychiatric care could help with your specific situation, learn more about how it works.
Mental Health Conditions Treated Through Virtual Psychiatric Care
Virtual psychiatric providers treat the full spectrum of mental health conditions. Here's a comprehensive overview of what conditions are addressed through telehealth:
Anxiety Disorders
Anxiety disorders are among the most common mental health conditions, affecting 40 million adults in the United States. Virtual psychiatric treatment is highly effective for anxiety management.
Generalized Anxiety Disorder (GAD): Persistent, excessive worry about multiple aspects of life (work, health, relationships, finances) that interferes with daily functioning. Physical symptoms include restlessness, fatigue, difficulty concentrating, muscle tension, and sleep problems.
Panic Disorder: Recurrent unexpected panic attacks with intense fear, heart palpitations, sweating, trembling, shortness of breath, and feelings of impending doom. Many people with panic disorder develop anxiety about having future panic attacks.
Social Anxiety Disorder: Intense fear of social situations where you might be judged, embarrassed, or scrutinized by others. This goes far beyond normal shyness and can severely limit work, school, and social participation.
Specific Phobias: Extreme fear of specific objects or situations (flying, heights, animals, medical procedures, blood) that leads to avoidance behavior.
Agoraphobia: Fear of places or situations where escape might be difficult or help unavailable if panic symptoms occur, often leading to avoidance of public spaces.
Treatment Approach: Psychiatric providers prescribe medications such as SSRIs (Zoloft, Lexapro, Prozac), SNRIs (Effexor, Cymbalta), benzodiazepines for short-term relief, and buspirone. Treatment often combines medication with therapy referrals for cognitive-behavioral therapy (CBT).
Depression and Mood Disorders
Depression affects how you feel, think, and handle daily activities. Virtual psychiatric care provides accessible treatment for all types of depressive disorders.
Major Depressive Disorder (MDD): Persistent feelings of sadness, hopelessness, loss of interest in activities you once enjoyed, changes in appetite and sleep, fatigue, difficulty concentrating, and sometimes thoughts of death or suicide.
Persistent Depressive Disorder (Dysthymia): Chronic depression lasting two years or longer. Symptoms may be less severe than major depression but are long-lasting and impact quality of life.
Postpartum Depression: Depression that develops after childbirth, far more serious than "baby blues," involving severe mood changes, anxiety, exhaustion, and difficulty bonding with your baby.
Seasonal Affective Disorder (SAD): Depression that follows seasonal patterns, typically beginning in fall/winter and improving in spring/summer, related to reduced sunlight exposure.
Treatment-Resistant Depression: Depression that hasn't responded adequately to multiple medication trials. Providers may recommend specialized medications, combination therapies, or referrals for additional treatments like TMS or ketamine therapy.
Treatment Approach: Medications include SSRIs, SNRIs, atypical antidepressants (Wellbutrin, Remeron), and sometimes augmentation strategies. Genetic testing (GeneSight) can help identify which medications your body metabolizes most effectively.
Bipolar Disorder
Bipolar disorder involves extreme mood swings between manic/hypomanic highs and depressive lows. Proper medication management is essential for stability.
Bipolar I Disorder: Characterized by manic episodes lasting at least seven days (or severe enough to require hospitalization) with or without depressive episodes. Mania involves elevated mood, increased energy, decreased need for sleep, racing thoughts, impulsive behavior, and sometimes psychotic features.
Bipolar II Disorder: Involves hypomanic episodes (less severe than full mania) alternating with major depressive episodes. Hypomania may feel productive or creative but still represents mood instability.
Cyclothymic Disorder: Chronic mood instability with numerous periods of hypomanic and depressive symptoms that don't meet full criteria for episodes but cause significant distress.
Treatment Approach: Mood stabilizers (lithium, Depakote, Lamictal), atypical antipsychotics (Abilify, Seroquel, Latuda), and careful monitoring. Antidepressants are used cautiously due to risk of triggering mania. Regular follow-ups ensure medication levels remain therapeutic and side effects are managed.
ADHD (Attention-Deficit/Hyperactivity Disorder)
ADHD affects both children and adults, impacting attention, focus, impulse control, and organization. Virtual psychiatric care is particularly effective for ADHD management.
Inattentive Type: Difficulty sustaining attention, frequent careless mistakes, trouble organizing tasks, easily distracted, forgetfulness in daily activities. Often diagnosed later because symptoms are less disruptive than hyperactive type.
Hyperactive-Impulsive Type: Fidgeting, difficulty staying seated, talking excessively, interrupting others, difficulty waiting turns, acting without thinking about consequences.
Combined Type: Both inattentive and hyperactive-impulsive symptoms present.
Adult ADHD: Many adults weren't diagnosed as children but struggle with focus, organization, time management, and completing tasks. ADHD symptoms often impact work performance, relationships, and daily functioning.
Treatment Approach: Stimulant medications (Adderall, Ritalin, Vyvanse, Concerta) or non-stimulant options (Strattera, Wellbutrin, Intuniv).
PTSD and Trauma-Related Disorders
Post-traumatic stress disorder develops after experiencing or witnessing traumatic events. Virtual psychiatric treatment helps manage PTSD symptoms through medication and supportive care.
PTSD Symptoms: Intrusive memories, flashbacks, nightmares about the trauma. Avoidance of reminders of the traumatic event. Negative changes in thoughts and mood. Hyperarousal including being easily startled, feeling on edge, difficulty sleeping, and angry outbursts.
Complex PTSD (CPTSD): Results from prolonged, repeated trauma (childhood abuse, domestic violence, long-term captivity). Involves PTSD symptoms plus difficulties with emotional regulation, self-concept, and relationships.
If you've experienced trauma and are struggling with symptoms that won't go away, you're not alone. Our providers understand trauma bonding, CPTSD, and how to break free from unhealthy patterns.
Acute Stress Disorder: Similar symptoms to PTSD but occurring within one month of trauma exposure and lasting less than one month.
Adjustment Disorders: Emotional or behavioral symptoms developing within three months of a significant life stressor (job loss, divorce, moving, illness) that cause distress disproportionate to the stressor.
Treatment Approach: SSRIs and SNRIs for PTSD symptoms, prazosin for nightmares, and medications for associated anxiety or depression. Psychiatric providers often coordinate with trauma-specialized therapists offering EMDR or trauma-focused CBT.
Obsessive-Compulsive Disorder (OCD)
OCD involves unwanted, intrusive thoughts (obsessions) and repetitive behaviors or mental acts (compulsions) performed to reduce anxiety caused by obsessions.
Common Obsessions:
- Contamination fears
- Intrusive violent or sexual thoughts
- Need for symmetry or exactness
- Religious or moral concerns
- Fear of harm coming to self or others
Common Compulsions:
- Excessive hand washing or cleaning
- Checking behaviors (locks, appliances, switches)
- Counting, repeating, or ordering rituals
- Mental compulsions (praying, counting, repeating phrases)
- Seeking reassurance repeatedly
Treatment Approach: SSRIs at higher doses than used for depression (Prozac, Zoloft, Luvox, Anafranil), sometimes augmented with atypical antipsychotics. Treatment works best when combined with exposure and response prevention (ERP) therapy.
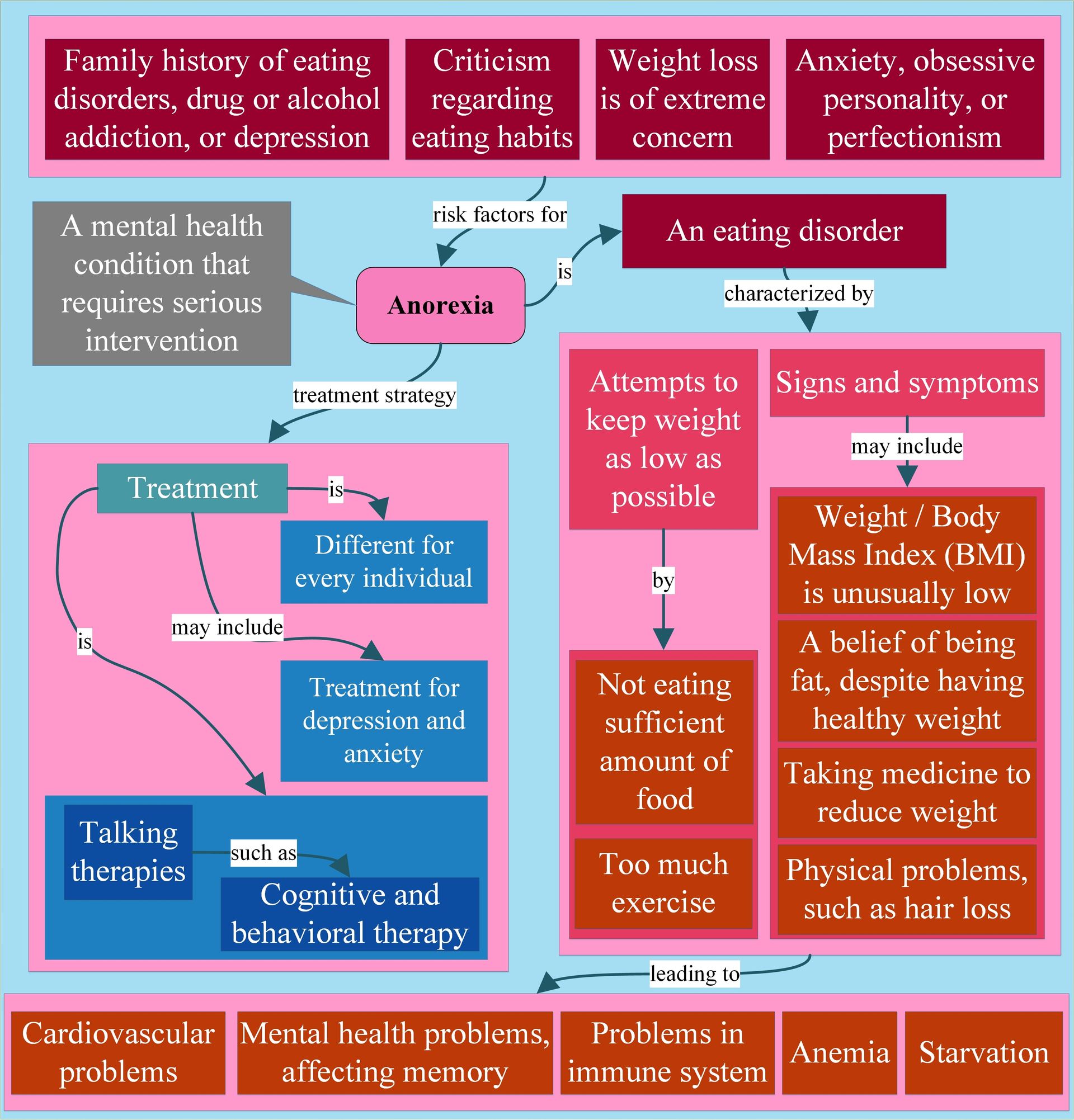
Eating Disorders
Eating disorders are serious mental health conditions involving disturbed eating patterns, body image issues, and intense fear of weight gain.
Anorexia Nervosa: Restricted food intake, intense fear of gaining weight, distorted body image, and dangerously low body weight.
Bulimia Nervosa: Cycles of binge eating followed by compensatory behaviors (purging, excessive exercise, fasting).
Binge Eating Disorder: Recurrent episodes of eating large quantities of food, feeling out of control during binges, without regular compensatory behaviors.
ARFID (Avoidant/Restrictive Food Intake Disorder): Limited food intake not related to body image concerns, often due to sensory issues, lack of interest in eating, or fear of adverse consequences.
Treatment Approach: SSRIs for associated anxiety and depression, sometimes Vyvanse for binge eating disorder. Psychiatric care coordinates with nutritionists, therapists specializing in eating disorders, and medical doctors monitoring physical health.
Psychotic Disorders
Psychotic disorders involve breaks from reality including hallucinations (seeing or hearing things others don't), delusions (fixed false beliefs), and disorganized thinking.
Schizophrenia: Chronic condition involving hallucinations, delusions, disorganized speech and behavior, reduced emotional expression, and decreased motivation.
Schizoaffective Disorder: Combination of schizophrenia symptoms with significant mood episodes (depression or mania).
Brief Psychotic Disorder: Sudden onset of psychotic symptoms lasting less than one month, often triggered by extreme stress.
Treatment Approach: Atypical antipsychotic medications (Abilify, Risperdal, Zyprexa, Seroquel, Latuda, Invega) with regular monitoring for effectiveness and side effects. Close coordination with case managers and therapists.
Insomnia and Sleep Disorders
Sleep problems often accompany mental health conditions or exist independently, significantly impacting quality of life.
Insomnia: Difficulty falling asleep, staying asleep, or waking too early with inability to return to sleep. Chronic insomnia persists at least three nights per week for three months or longer.
Treatment Approach: Medications may include trazodone, mirtazapine, gabapentin, or short-term use of sleep aids like Ambien or Lunesta. Providers emphasize sleep hygiene education and addressing underlying conditions contributing to insomnia.
Substance Use Disorders
Psychiatric providers offer medication-assisted treatment (MAT) for substance use disorders, particularly opioid and alcohol use disorders.
Opioid Use Disorder: Addiction to opioids (heroin, prescription painkillers) treated with medications like buprenorphine (Suboxone, Subutex) that reduce cravings and withdrawal symptoms.
Alcohol Use Disorder: Problematic alcohol use treated with medications like naltrexone, acamprosate, or disulfiram alongside counseling and support groups.
Treatment Approach: Medication-assisted treatment combined with therapy, support groups, and monitoring. Virtual care removes barriers to accessing MAT in underserved areas.
Personality Disorders
Personality disorders involve enduring patterns of thoughts, feelings, and behaviors that differ significantly from cultural expectations and cause distress or impairment.
Borderline Personality Disorder (BPD): Intense, unstable relationships, fear of abandonment, impulsivity, emotional instability, chronic feelings of emptiness, and sometimes self-harm or suicidal behavior.
Understanding relationship patterns is crucial for healing. If you struggle with relationship dynamics, learn about why empaths and narcissists attract each other and how to tell the difference between avoidant attachment and narcissistic traits.
Treatment Approach: Medications targeting specific symptoms like mood instability (mood stabilizers), impulsivity (SSRIs), or brief psychotic symptoms (low-dose antipsychotics). Dialectical behavior therapy (DBT) is the gold-standard therapy for BPD.
Women's Mental Health Issues
Psychiatric care addresses mental health concerns specific to women's reproductive cycles and life stages.
Premenstrual Dysphoric Disorder (PMDD): Severe mood changes, irritability, depression, and anxiety in the week or two before menstruation that significantly impact functioning.
Perinatal Mental Health: Depression and anxiety during pregnancy or postpartum period requiring careful medication selection safe for pregnancy and breastfeeding.
Menopause-Related Mood Changes: Depression, anxiety, irritability, and sleep problems related to hormonal changes during perimenopause and menopause.
Treatment Approach: SSRIs, hormone considerations, lifestyle interventions, and close monitoring during pregnancy and postpartum periods.
Child and Adolescent Psychiatry
Virtual psychiatric care serves children and adolescents experiencing mental health challenges.
Conditions Treated:
- ADHD
- Anxiety disorders
- Depression
- Behavioral issues
- Autism spectrum disorder (screening and medication management)
- Trauma and stress-related disorders
- Eating disorders
- Mood disorders
Treatment Approach: Age-appropriate medication management with careful consideration of developing brains and bodies. Strong emphasis on parent education, school coordination, and therapy referrals.
LGBTQ+ Mental Health
Providers offer affirming, inclusive care for LGBTQ+ individuals addressing unique mental health challenges.
Common Concerns:
- Depression and anxiety related to discrimination, stigma, or identity struggles
- Gender dysphoria
- Trauma from rejection or violence
- Substance use
- Relationship challenges
Treatment Approach: Culturally competent, affirming psychiatric care that respects identity and addresses both general mental health needs and LGBTQ+-specific concerns.
Geriatric Psychiatry
Specialized psychiatric care for older adults addresses mental health conditions common in aging populations.
Conditions Addressed:
- Late-life depression
- Anxiety in older adults
- Dementia-related behavioral symptoms
- Sleep disorders
- Adjustment to life transitions (retirement, loss, health changes)
Treatment Approach: Careful medication selection considering multiple medical conditions, drug interactions, and age-related changes in medication metabolism.
If you're looking for comprehensive information about all conditions Virtual Psychiatric Care treats, visit the
What We Treat page.
Psychiatric Medications: What to Expect
Understanding psychiatric medications helps you feel more confident about treatment. Here's what you need to know about the most common medication classes:
Antidepressants
Antidepressants treat depression, anxiety disorders, OCD, PTSD, and some chronic pain conditions.
SSRIs (Selective Serotonin Reuptake Inhibitors): Most commonly prescribed antidepressants. Examples: Zoloft (sertraline), Lexapro (escitalopram), Prozac (fluoxetine), Celexa (citalopram), Paxil (paroxetine).
How they work: Increase serotonin levels in the brain, improving mood and reducing anxiety.
Timeline: May take 4-6 weeks to feel full effects. Start low and increase gradually to minimize side effects.
Common side effects: Nausea, headache, sleep changes, sexual side effects. Most side effects improve after the first few weeks.
SNRIs (Serotonin-Norepinephrine Reuptake Inhibitors): Examples: Effexor (venlafaxine), Cymbalta (duloxetine), Pristiq (desvenlafaxine).
How they work: Increase both serotonin and norepinephrine, helpful for depression with low energy and chronic pain conditions.
Timeline and side effects: Similar to SSRIs.
Atypical Antidepressants: Examples: Wellbutrin (bupropion), Remeron (mirtazapine), Trintellix (vortioxetine).
Wellbutrin: Increases dopamine and norepinephrine. Doesn't cause sexual side effects or weight gain. Often used for depression with fatigue or to help with smoking cessation.
Remeron: Increases serotonin and norepinephrine. Helpful for depression with insomnia and poor appetite. Can cause increased appetite and drowsiness.
Anti-Anxiety Medications
Benzodiazepines: Examples: Xanax (alprazolam), Klonopin (clonazepam), Ativan (lorazepam), Valium (diazepam).
How they work: Rapid relief of acute anxiety symptoms by enhancing GABA (calming neurotransmitter).
Usage: Typically prescribed short-term or as-needed due to tolerance and dependence risk. Very effective for panic attacks, acute anxiety, and sleep.
Important considerations: Can be habit-forming with long-term use. Shouldn't be stopped abruptly. Not recommended as first-line treatment for chronic anxiety.
Buspirone: Non-benzodiazepine anti-anxiety medication. Takes several weeks to work. No addiction potential. Helpful for generalized anxiety disorder.
Hydroxyzine (Vistaril): Antihistamine with anti-anxiety properties. Works quickly, non-addictive. Used as needed for anxiety or sleep.
Mood Stabilizers
Used primarily for bipolar disorder to prevent mood episodes.
Lithium: Gold-standard mood stabilizer. Highly effective for bipolar disorder. Requires regular blood tests to monitor therapeutic levels and kidney/thyroid function.
Anticonvulsant Mood Stabilizers: Examples: Depakote (valproic acid), Lamictal (lamotrigine), Tegretol (carbamazepine).
Lamictal: Particularly effective for bipolar depression. Requires slow dose increase to avoid rare but serious rash.
Depakote: Effective for mania. Requires blood level monitoring.
Antipsychotic Medications
Treat psychotic disorders, bipolar disorder, and sometimes used to augment antidepressants for treatment-resistant depression.
Atypical (Second-Generation) Antipsychotics: Examples: Abilify (aripiprazole), Seroquel (quetiapine), Zyprexa (olanzapine), Risperdal (risperidone), Latuda (lurasidone), Rexulti (brexpiprazole).
Uses: Schizophrenia, bipolar disorder, augmentation for depression, severe anxiety, agitation.
Monitoring: Regular metabolic monitoring (weight, blood sugar, cholesterol) as some antipsychotics can affect metabolism.
ADHD Medications
Stimulants: Examples: Adderall (amphetamine), Ritalin/Concerta (methylphenidate), Vyvanse (lisdexamfetamine).
How they work: Increase dopamine and norepinephrine, improving focus, attention, and impulse control.
Forms: Immediate-release (lasts 4-6 hours) or extended-release (lasts 8-12 hours).
Common side effects: Decreased appetite, difficulty sleeping, increased heart rate. Usually managed with timing of doses and lifestyle adjustments.
Non-Stimulant ADHD Medications: Examples: Strattera (atomoxetine), Intuniv (guanfacine), Kapvay (clonidine).
Benefits: No abuse potential, smooth effect throughout day, helpful when stimulants cause side effects or for people with substance use history.
Drawbacks: Take longer to work (2-4 weeks), may be less effective than stimulants for some people.
Sleep Medications
Common Prescriptions:
● Trazodone: Sedating antidepressant, very commonly used off-label for insomnia
● Ambien (zolpidem): Short-acting sleep aid
● Lunesta (eszopiclone): Sleep aid
● Belsomra (suvorexant): Newer mechanism, blocks wakefulness signals
● Remeron: Antidepressant with strong sedating effects
Approach: Providers emphasize sleep hygiene (consistent schedule, limiting screens, cool dark room) alongside medication. Many sleep medications are intended for short-term use while addressing underlying causes.
Medication for Substance Use Disorders
Buprenorphine (Suboxone, Subutex): Treats opioid use disorder by reducing cravings and withdrawal symptoms without producing euphoria. Allows people to stabilize their lives while in recovery.
Naltrexone: Blocks opioid receptors (for opioid use disorder) or reduces alcohol cravings (for alcohol use disorder). Available as daily pill (ReVia) or monthly injection (Vivitrol).
Acamprosate (Campral): Reduces alcohol cravings by normalizing brain chemistry affected by chronic alcohol use.
How Medication Management Works Virtually
Initial Evaluation: Your provider takes comprehensive history, discusses symptoms, reviews previous medications tried, and considers your preferences and concerns. Together you decide on the best medication to start.
Starting Medication: Typically begin with low doses and increase gradually to minimize side effects while finding the effective therapeutic dose.
Follow-Up Schedule:
First Month: Follow-up appointments every 1-2 weeks to assess response, side effects, and make any needed adjustments.
After Stabilization: Appointments typically every 1-3 months for ongoing medication management and monitoring.
Between Appointments: Secure messaging through patient portal for questions, concerns, or needed adjustments.
Monitoring: Some medications require periodic lab work (lithium levels, liver function, kidney function, metabolic panels). Your provider orders labs you can complete at local facilities, then reviews results virtually.
Medication Adjustments: If medication isn't working well or causes problematic side effects, your provider adjusts the dose or tries different medications. This is a collaborative process to find what works best for you.
GeneSight Genetic Testing
Virtual Psychiatric Care offers optional GeneSight pharmacogenomic testing that analyzes your DNA to determine how your body metabolizes psychiatric medications.
How It Works: A DNA swab kit ships to your home. You complete the oral swab and mail it back in a prepaid envelope. Results are ready in a few days.
What It Reveals: Which medications you're likely to metabolize normally, slowly, or rapidly. This helps providers choose medications most likely to work well for you with fewest side effects.
Benefits: Less trial-and-error with medications. Faster path to effective treatment. Reduced risk of side effects from medications your body doesn't process well.
Cost: With commercial insurance, maximum cost is $330 (often divided into payment plan). Financial assistance available, potentially as low as $0 copay.
Learn more about what we treat and specialized services including GeneSight testing.
What to Expect From Your Virtual Psychiatric Appointments
Understanding what happens during virtual psychiatric appointments helps you feel prepared and confident.
Your First Appointment: The Psychiatric Evaluation
How Long It Takes: Initial psychiatric evaluations at Virtual Psychiatric Care last 45-60 minutes, giving enough time for thorough assessment.
What Your Provider Will Ask:
Current Symptoms: What brings you to seek psychiatric care? What symptoms are you experiencing? How long have you been struggling? How do symptoms impact your daily life, work, relationships, and functioning?
Mental Health History: Previous diagnoses, medications tried and their effectiveness, therapy history, previous hospitalizations or intensive treatment, family history of mental health conditions.
Medical History: Current medical conditions, medications, allergies, recent lab work, substance use (alcohol, marijuana, other drugs).
Social History: Living situation, relationships, work or school, support system, trauma history, current stressors.
Safety Assessment: Thoughts of harming yourself or others, past suicide attempts, current safety and support.
Goals for Treatment: What do you hope to achieve through psychiatric treatment? What would improvement look like for you?
What Happens Next:
Diagnosis: Your provider explains their clinical assessment and diagnosis based on your symptoms and history.
Treatment Recommendations: Discussion of treatment options including medications, therapy, lifestyle changes, and other interventions.
Medication Decision: If medication is recommended, your provider explains which medication they suggest, how it works, potential side effects, what to expect, and answers your questions.
Treatment Plan: Together you create a plan including starting medication (if appropriate), follow-up schedule, and any additional recommendations (therapy referral, lifestyle changes, lab work).
Prescription: If you agree to medication, your provider sends it electronically to your pharmacy during or immediately after the appointment.
Follow-Up: Schedule your next appointment before leaving the video session.
Follow-Up Appointments
Duration: Typically 15-30 minutes depending on complexity and what needs to be addressed.
What's Covered:
Medication Response: How are you feeling? Is the medication helping? To what extent have symptoms improved?
Side Effects: Any unwanted effects? Are they manageable or problematic?
Dose Adjustments: Based on your response and any side effects, does the dose need to be increased, decreased, or kept the same?
Medication Changes: If current medication isn't working well, discuss trying a different medication or adding something.
Refills: Ensure prescriptions are refilled and sent to pharmacy.
Overall Functioning: How are you managing day-to-day? Work? Relationships? Sleep? Mood? Energy?
Questions and Concerns: Opportunity to discuss anything on your mind about treatment.
Technology Requirements
Virtual psychiatric appointments require minimal technology:
Devices: Any smartphone, tablet, or computer with camera and microphone. Both Apple and Android devices work.
Internet: Reliable internet connection (WiFi or cellular data). Video quality adjusts automatically based on connection speed.
Software: Free VSee Clinic app available for download on App Store and Google Play. No special software needed beyond the app.
Privacy: HIPAA-compliant, secure, encrypted video platform protecting your privacy and health information.
Technical Support: If you experience any technical difficulties, support is available to help you connect successfully.
Scheduling and Access
Flexible Hours: Appointments available Monday through Friday 9am to 9pm EST, Saturday 12pm to 3pm EST.
Same-Day Appointments: Walk-in option allows you to enter virtual waiting room for same-day appointments based on provider availability.
Scheduled Appointments: Book future appointments at specific times convenient for your schedule.
Free Pre-Appointment Chat: Option to message provider with questions before booking to ensure good fit.
How Long Until First Appointment: New patients can often be seen within days, sometimes same day, unlike traditional psychiatry where wait times are often weeks or months.
To learn about the specific process for booking, visit How It Works.
Benefits of Virtual Psychiatric Treatment
Virtual psychiatric care offers significant advantages over traditional in-person appointments:
Convenience and Accessibility
No Travel: Attend appointments from home, work, car, or any private location. Save time and money on transportation.
No Waiting Rooms: Log in from your private space rather than sitting in medical office waiting rooms.
Fits Your Schedule: Evening and weekend hours available. Easier to fit appointments around work, childcare, and other commitments.
Geographic Access: Access psychiatric care even if you live in rural areas or locations without local psychiatrists. Virtual Psychiatric Care serves patients in over 40 states.
Privacy and Comfort
Your Environment: Meet with your provider from wherever you feel most comfortable and relaxed.
Reduced Stigma: Some people feel less anxious about seeking mental health treatment when they don't have to visit a psychiatric office.
Discretion: Easier to keep appointments private without explaining office visits or taking obvious time off work.
Faster Access to Care
Shorter Wait Times: Traditional psychiatry often has 4-8 week wait times for new patients. Virtual providers can often see you within days.
Same-Day Options: Walk-in appointments available for urgent needs.
Continuity During Life Changes: If you move, travel for work, or have changing circumstances, virtual care continues seamlessly without finding new providers.
Quality and Effectiveness
Same Standard of Care: Virtual psychiatric evaluations and medication management provide the same clinical quality as in-person care.
Licensed Professionals: All providers are fully licensed psychiatrists or psychiatric-mental health nurse practitioners.
Research-Backed: Extensive evidence shows virtual psychiatric care produces equivalent outcomes to in-person care for most conditions.
Better Adherence: Convenience of virtual appointments may actually improve treatment adherence, as people are more likely to attend appointments that don't require travel.
Cost-Effectiveness
Lower Costs: Virtual care often costs less than in-person appointments.
Insurance Accepted: Most major insurance plans cover virtual psychiatric care at the same rates as in-person care.
Self-Pay Options: Transparent, affordable self-pay rates for those without insurance or who prefer not to use insurance.
No Hidden Costs: No parking fees, transportation costs, or time off work.
For detailed information about costs and insurance, visit Insurance & Fees.
Getting Started with Virtual Psychiatric Care
Ready to begin treatment? Here's how to get started:
For Self-Pay Patients
Step 1: Book Your Appointment Click "Book Now" on the Virtual Psychiatric Care website. Choose your state and preferred provider.
Step 2: Choose Appointment Type Select "Enter Waiting Room" for same-day walk-in appointments, or "Book Appointment" to schedule a future date and time.
Step 3: Create Account Set up your patient portal account and complete intake forms with information about your symptoms, history, and current medications.
Step 4: Download App Download the free VSee Clinic app on your smartphone or tablet for easiest access (or use web browser on computer).
Step 5: Enter Payment Provide payment method for authorization hold. Card is NOT charged until after your completed appointment.
Step 6: Attend Appointment Join your video appointment at scheduled time using the link sent via text and email.
For Insured Patients
Step 1: Request Appointment Click "Book Now Insured" button on the website.
Step 2: Complete Portal Forms Welcome email sent within 24 hours with link to complete required intake forms in patient portal.
Step 3: Verification Virtual Psychiatric Care verifies your insurance benefits and approves your appointment request.
Step 4: Confirmation Receive appointment confirmation with date, time, and video call link.
Step 5: Attend Appointment Log into patient portal at scheduled time to begin video call with your provider.
Insurance Questions: Call 786-761-1155 to inquire about using in-network or out-of-network benefits.
What to Prepare Before Your First Appointment
List Current Medications: Write down all medications you're currently taking (including over-the-counter and supplements) with doses.
Symptom Timeline: Note when symptoms started, how they've progressed, and what makes them better or worse.
Previous Treatment: List any psychiatric medications you've tried in the past, how long you took them, whether they helped, and any side effects experienced.
Current Struggles: Think about specific ways symptoms impact your life (sleep, work, relationships, daily activities).
Questions: Write down any questions you want to ask your provider.
Private Space: Ensure you'll be in a private location where you can talk openly without being overheard.
Good Connection: Make sure you have reliable internet (WiFi or cellular data strong enough for video).
After Your Appointment
Prescription Pickup: Your pharmacy will notify you when your prescription is ready (usually same day or next day).
Start Medication: Follow your provider's instructions about when and how to take your medication.
Note Changes: Pay attention to how you feel, any side effects, and what's improving so you can report at follow-up.
Follow-Up Appointment: Attend your scheduled follow-up (typically 1-2 weeks after starting medication).
Portal Access: Use patient portal for secure messaging with provider between appointments if questions arise.
For detailed answers to common questions, visit the FAQs page.
When to Seek Psychiatric Help
How do you know if you need psychiatric treatment? Here are signs it's time to reach out:
Symptoms Significantly Impact Your Life
Work or School Performance Suffering: Difficulty concentrating, completing tasks, meeting deadlines, or functioning at your usual level.
Relationship Problems: Mood changes, irritability, withdrawal, or behaviors straining relationships with family, friends, or partners.
Daily Activities Affected: Struggling with basic self-care, household tasks, or activities you previously managed easily.
Physical Symptoms: Sleep problems, appetite changes, fatigue, physical tension, or other symptoms without clear medical cause.
Symptoms Persist Despite Your Efforts
Self-Help Hasn't Helped: You've tried exercise, sleep improvement, stress management, and other strategies but symptoms continue.
Getting Worse: Symptoms are intensifying or new symptoms are developing.
Lasting Weeks or Months: Brief periods of sadness or anxiety are normal. Symptoms persisting for weeks to months suggest clinical condition needing treatment.
Your Safety or Others' Safety Is at Risk
Thoughts of Self-Harm: Any thoughts of hurting yourself, suicide ideation, or self-destructive urges require immediate professional help.
Thoughts of Harming Others: Thoughts of violence toward others need urgent intervention.
Risky Behaviors: Impulsive, dangerous, or reckless behaviors that could result in harm.
Crisis Resources: If you're in immediate crisis, call 988 (Suicide and Crisis Lifeline), text HOME to 741741 (Crisis Text Line), or go to your nearest emergency room. Visit Crisis Resources for additional support.
Previous Treatment Hasn't Been Enough
Therapy Alone Isn't Enough: You're working with a therapist but symptoms persist or worsen, suggesting medication might help.
Primary Care Medications Aren't Working: Your family doctor prescribed an antidepressant but you're not improving, need specialized expertise, or require multiple medications.
Complex Symptoms: You have multiple mental health conditions requiring specialized psychiatric management.
Specific Condition Indicators
Depression: Persistent sadness, loss of interest in activities, hopelessness, worthlessness, changes in sleep/appetite lasting two weeks or more.
Anxiety: Excessive worry, panic attacks, avoidance of situations, physical anxiety symptoms interfering with life.
ADHD: Lifelong pattern of inattention, hyperactivity, or impulsivity significantly impacting multiple life areas.
Mood Swings: Extreme highs and lows, impulsive behavior during "up" periods, deep depression during "down" periods.
Trauma Symptoms: Nightmares, flashbacks, hypervigilance, avoidance, or emotional numbness after traumatic experiences.
Psychotic Symptoms: Hallucinations, delusions, disorganized thinking, or breaks from reality.
Understanding the Difference: Psychiatrist vs. Therapist
Many people wonder about the difference between psychiatrists and therapists. Understanding this helps you seek the right type of care.
Psychiatrists and Psychiatric Nurse Practitioners
Training: Psychiatrists are medical doctors (MD or DO) who completed medical school plus 4-year psychiatry residency. Psychiatric-Mental Health Nurse Practitioners (PMHNPs) are registered nurses with advanced practice degrees specializing in psychiatric care.
What They Do:
- Diagnose mental health conditions
- Prescribe and manage psychiatric medications
- Order and interpret medical tests
- Provide some therapy but primarily focus on medication management
When to See Them: When you need medication for mental health conditions, have complex psychiatric needs, or need medical expertise in mental health.
To learn more about the difference, read Psychiatrist vs. PMHNP: What's the Difference?
Therapists and Counselors
Training: Psychologists (PhD or PsyD), Licensed Clinical Social Workers (LCSW), Licensed Professional Counselors (LPC), or Marriage and Family Therapists (LMFT) with master's or doctoral degrees in mental health fields.
What They Do:
- Provide talk therapy and counseling
- Teach coping strategies
- Help process emotions and experiences
- Address relationship and behavioral issues
- CANNOT prescribe medication (except in a few states where psychologists have limited prescribing authority)
When to See Them: For talk therapy, processing trauma, developing coping skills, working through life challenges, or addressing relationship issues.
Combined Treatment: Best of Both Worlds
The Most Effective Approach: Research shows that for many conditions, combining medication management (from psychiatrist/PMHNP) with therapy (from therapist) produces better outcomes than either alone.
How It Works: You see a psychiatrist or PMHNP for medication management and a therapist for regular talk therapy. The providers can coordinate your care.
Virtual Psychiatric Care's Role: Provides the medication management component and can refer you to therapists for the counseling component of treatment.
FAQs About Virtual Psychiatric Treatment
Take the First Step Toward Better Mental Health
You don't have to struggle alone. Virtual psychiatric treatment makes getting help easier, more convenient, and more accessible than ever before.
Whether you're dealing with anxiety that won't go away, depression weighing you down, ADHD making life harder than it should be, or any other mental health challenge, effective treatment is available.
Getting started is simple:
Call: 786-761-1155
Email: Support@VirtualPsychiatricCare.com
Book Online:
Schedule your appointment for insured patients or
book self-pay appointment
Free pre-appointment chat available with providers to answer questions before booking.
Resources:
You deserve to feel better. Take the first step today.
Virtual Psychiatric Care
Accessible, Effective Virtual Psychiatric Treatment
Contact Us | Book Appointment | What We Treat | How It Works
Disclaimer: The information provided on this blog is for general informational purposes only and is not intended as, and should not be considered, medical advice. All information, content, and material available on this blog are for general informational purposes only. Readers are advised to consult with a qualified healthcare professional for medical advice, diagnosis, or treatment. The author and the blog disclaim any liability for the decisions you make based on the information provided. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.